People today spend countless hours hunched over screens, which strains the delicate structures connecting the neck to the head. This common habit triggers intense discomfort that radiates upward. Severe neck pain and headache base of skull disrupts sleep, work, and overall quality of life for millions worldwide. Experts link these symptoms to muscle tension, nerve irritation, and joint issues in the upper cervical region. Individuals who ignore early signs often face prolonged recovery times, so proactive awareness becomes essential for lasting relief.
The suboccipital muscles at the back of the neck play a critical role in head movement and posture stability. When these muscles tighten from prolonged forward head tilt, they compress nearby nerves and blood vessels. Patients notice sharp or throbbing sensations that start low and climb toward the scalp. Medical professionals emphasize that early intervention prevents escalation into chronic conditions like cervicogenic headaches.
The Anatomy Behind the Discomfort
The cervical spine consists of seven vertebrae that support the head’s weight while allowing flexible motion. Nerves called the greater and lesser occipital nerves emerge from the upper neck and travel to the base of the skull. Any irritation here sends pain signals directly to the head. Bone spurs from wear and tear or inflamed joints further aggravate the area. Doctors examine these structures through physical tests and imaging to pinpoint exact sources of distress. Understanding this anatomy helps patients visualize why simple posture changes yield dramatic improvements in daily comfort.
Primary Causes of Severe Neck Pain and Headache Base of Skull
Poor posture ranks as the top contributor to upper neck strain in modern lifestyles. Office workers and smartphone users develop forward head posture that overloads the suboccipital muscles. Severe neck pain and headache base of skull often stems from this mechanical imbalance. Whiplash injuries from car accidents jolt the cervical spine and inflame soft tissues. Herniated discs between C1 and C2 vertebrae pinch nerves that refer pain upward. Arthritis in the facet joints causes inflammation that radiates to the skull base. Occipital neuralgia develops when tight muscles or bone changes compress the occipital nerves. Infections or rare tumors also trigger similar patterns, though physicians rule these out quickly through targeted exams.
Degenerative changes accumulate over years and accelerate with age or repetitive stress. Rheumatoid arthritis inflames joint linings and erodes cartilage. Diabetes or gout heightens nerve sensitivity in some cases. Tight neck muscles from emotional stress trap nerves and restrict blood flow. Each cause demands tailored approaches because generic treatments fail to address root mechanisms.
Recognizing the Symptoms
Patients describe the pain as electric shocks or constant throbbing that worsens with neck rotation or prolonged sitting. Stiffness limits head turning, and tenderness appears when pressing the skull base. Light sensitivity and nausea sometimes accompany the episodes, mimicking migraines yet originating from the neck. One-sided pain that shoots toward the eyes or forehead signals nerve involvement. Scalp tenderness makes brushing hair or wearing hats uncomfortable. These symptoms persist for hours or days unless addressed promptly.
Associated issues include shoulder tightness, blurred vision during flares, and disrupted sleep from discomfort. Individuals report reduced concentration at work because the constant ache drains mental energy. Tracking symptom patterns helps doctors differentiate cervicogenic headaches from primary types like tension or cluster headaches.
Diagnostic Approaches
Physicians begin with detailed medical histories that explore recent injuries, work habits, and lifestyle factors. Physical exams test neck range of motion and palpate for trigger points at the skull base. Imaging studies such as X-rays reveal bone spurs or alignment issues. MRI scans provide clear views of soft tissues, discs, and nerves. CT scans offer precise cross-sections when bone details matter most. Nerve block injections serve dual purposes by confirming diagnoses and delivering immediate relief. Blood tests rule out inflammatory or infectious causes in complex cases.
Specialists collaborate to exclude serious conditions like meningitis or vascular problems. Accurate diagnosis guides effective treatment plans and prevents unnecessary procedures.
Immediate Home Relief Strategies
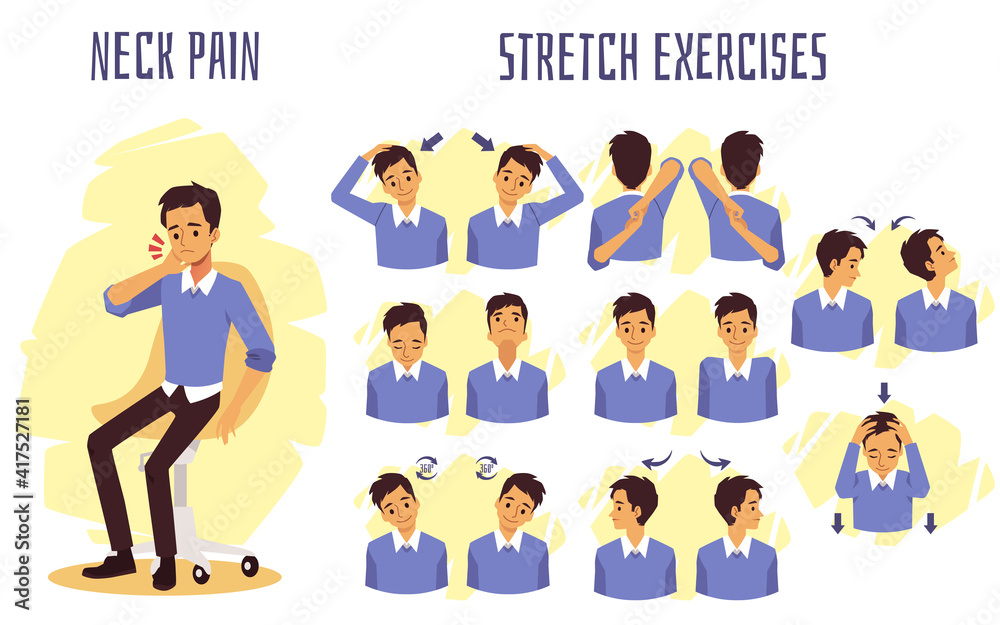
Heat therapy relaxes tight muscles and improves blood circulation around the upper neck. Patients apply warm compresses for 15 minutes several times daily to ease stiffness. Cold packs reduce inflammation during acute flares and numb sharp sensations. Gentle stretches target the suboccipital group and restore mobility without strain. Chin tucks strengthen deep neck flexors while countering forward posture. Shoulder rolls release upper trapezius tension that contributes to referred head pain.
Over-the-counter anti-inflammatory medications provide short-term relief when used as directed. Hydration supports tissue health and prevents dehydration-triggered exacerbations. Ergonomic adjustments at desks maintain neutral spine alignment and reduce daily strain. Massage techniques applied to the neck and scalp release myofascial restrictions. These methods empower individuals to manage symptoms independently while awaiting professional evaluation.
Professional Medical Interventions
Physical therapy programs strengthen supporting muscles and correct biomechanical faults. Therapists guide patients through progressive exercises that improve posture and nerve gliding. Manual therapy techniques mobilize stiff joints and release muscle knots. Prescription muscle relaxants calm spasms in severe episodes. Anticonvulsant medications stabilize overactive nerves in occipital neuralgia cases. Steroid injections around inflamed nerves deliver targeted anti-inflammatory effects. In persistent situations, radiofrequency ablation disrupts pain signals from specific nerves.
Surgical options remain rare but address severe disc herniations or structural compression. Multidisciplinary teams combine interventions for optimal outcomes. Patients who follow customized plans experience significant reductions in frequency and intensity of episodes.
Preventive Measures and Lifestyle Adjustments
Consistent posture awareness during screen time prevents muscle overload. Individuals set reminders to check alignment and perform micro-breaks every 30 minutes. Regular exercise routines that include yoga or swimming build neck resilience and enhance flexibility. Stress management techniques such as meditation lower overall muscle tension. Supportive pillows maintain neutral neck positions during sleep and reduce morning stiffness. Weight management decreases load on the cervical spine. Smoking cessation improves circulation and accelerates tissue healing.
Workplace ergonomics play a pivotal role in long-term prevention. Adjustable chairs, monitor heights at eye level, and keyboard positioning keep the head balanced over the shoulders. These habits compound over time to minimize recurrence risks.
Severe neck pain and headache base of skull demands attention when accompanied by fever, vision changes, or sudden weakness. Individuals seek immediate care if pain follows head trauma or persists despite home measures. Early professional input avoids complications and restores function faster.
When Professional Help Becomes Essential
Severe neck pain and headache base of skull signals potential nerve compression that requires prompt evaluation. Numbness in the arms, dizziness, or coordination loss indicates urgent assessment. Physicians recommend imaging when symptoms intensify rapidly or interfere with daily activities. Ongoing pain beyond two weeks despite conservative care warrants specialist referral. Multidisciplinary clinics offer comprehensive evaluations that integrate neurology, orthopedics, and rehabilitation expertise.
Patients who partner actively with healthcare providers achieve better long-term control and resume normal routines confidently.
Long-Term Management and Outlook
Successful management combines daily habits with occasional professional support. Individuals who maintain strong core and neck muscles report fewer flares. Nutritional choices rich in anti-inflammatory foods support joint health and reduce systemic inflammation. Community support groups connect people facing similar challenges and share practical tips. Ongoing research into nerve modulation techniques promises even more effective options in coming years.
Severe neck pain and headache base of skull affects people across all ages, yet targeted strategies deliver reliable relief. Consistent application of prevention principles transforms discomfort into manageable episodes. Patients regain control by addressing root causes rather than masking symptoms.
Conclusion
Active participation in neck health yields transformative results for those plagued by upper cervical issues. Education about anatomy and triggers empowers informed decisions. Healthcare advancements continue to refine diagnostic precision and treatment efficacy. Individuals who prioritize posture, movement, and stress reduction enjoy sustained comfort and vitality. This guide equips readers with actionable knowledge to confront discomfort head-on and reclaim daily freedom from pain.
READ ALSO: Bile Duct Obstruction Symptoms: Complete Guide to Causes, Signs, and Treatment

