What Are the Chances of Surviving a Brain Bleed
Doctors diagnose brain bleeds, also known as intracranial hemorrhages, as life-threatening emergencies where blood escapes from damaged vessels and pools inside the skull. This buildup compresses brain tissue, cuts off oxygen supply, and triggers rapid swelling that demands immediate intervention.
Patients who reach emergency care quickly benefit from advanced imaging and targeted therapies that stabilize vital functions and limit damage. Medical teams monitor blood pressure, reverse clotting issues, and prepare for surgery when necessary because every minute counts in preserving brain cells. Families play a key role by recognizing early warning signs and seeking help without delay.
Understanding Brain Bleeds and Why They Strike Suddenly
Hypertension forces blood vessels to weaken over time and rupture under pressure, while trauma from falls or accidents tears delicate arteries near the brain surface. Aneurysms balloon outward and burst without warning, and blood-thinning medications increase leakage risk in vulnerable patients.
Amyloid angiopathy deposits proteins in older adults’ vessel walls and makes them brittle, leading to spontaneous bleeds in the brain lobes. Doctors identify these root causes through detailed history and lab tests so they can tailor treatment and prevent recurrence. Lifestyle factors like smoking, heavy alcohol use, and uncontrolled diabetes accelerate vessel damage and raise overall risk dramatically.
Different Types of Brain Bleeds Demand Specific Responses
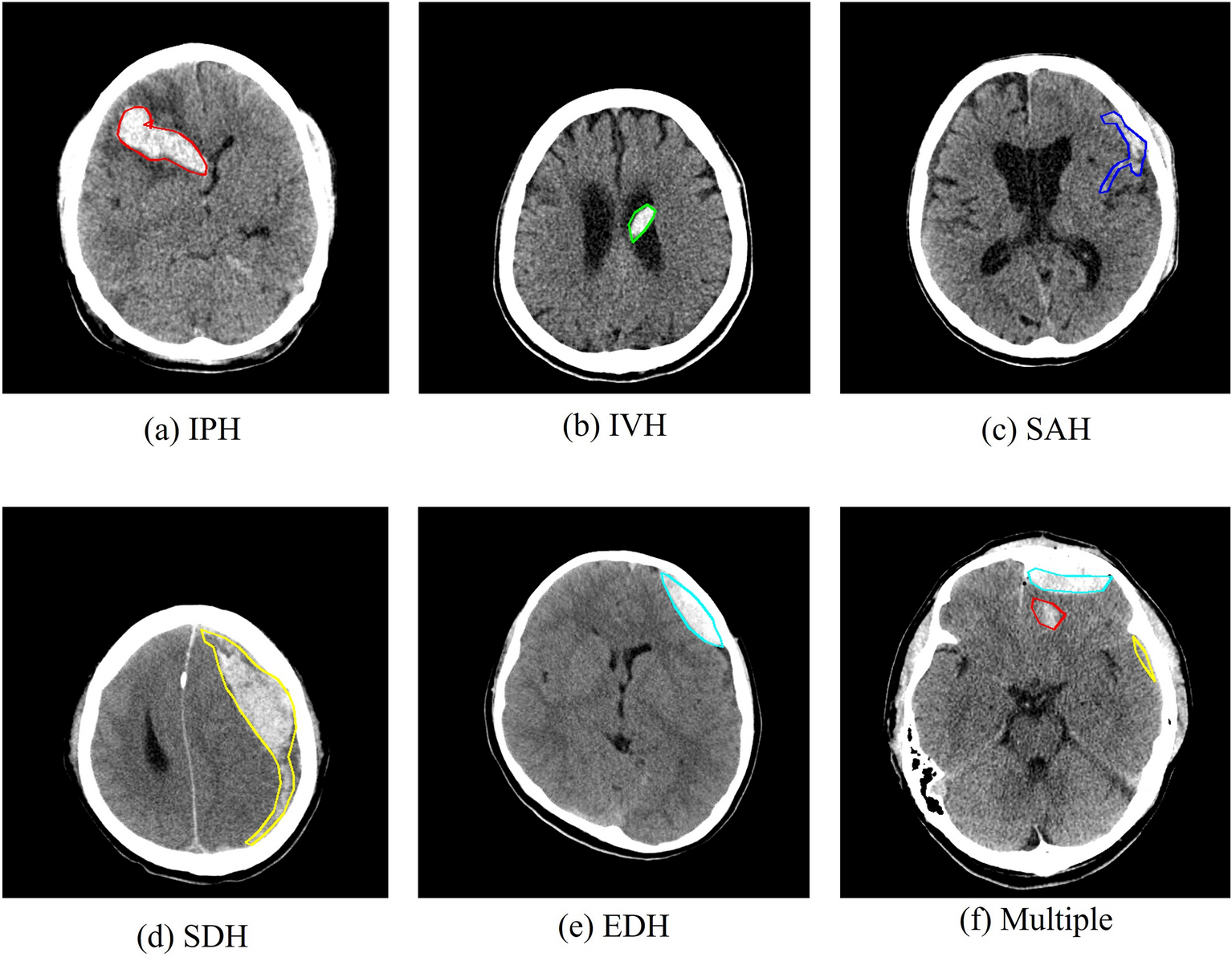
Epidural hematomas form between the skull and outer brain covering after head injury and expand rapidly, requiring urgent surgical evacuation. Subdural hematomas accumulate more slowly under the dura and affect elderly patients or those on anticoagulants, often needing drainage procedures. Subarachnoid hemorrhages flood the space around the brain after aneurysm rupture and cause severe headaches with neck stiffness that alert physicians immediately.
Intracerebral hemorrhages bleed directly into brain tissue and destroy functional areas, while intraventricular bleeds fill the fluid-filled chambers and block cerebrospinal flow. Each location influences symptoms, treatment urgency, and long-term effects that specialists evaluate case by case.
Recognizing Symptoms That Save Lives
Sudden intense headaches strike like thunderclaps and signal vessel rupture in many patients who describe the worst pain of their lives. One-sided weakness, numbness, or paralysis appears as the bleed presses on motor pathways and disrupts signals to limbs. Vision blurs or doubles, speech slurs, and confusion sets in when blood affects language or cognitive centers. Nausea, vomiting, seizures, and loss of consciousness follow as pressure builds inside the skull and threatens vital centers. Caregivers who act on these signs get patients to stroke centers faster and improve every survival metric doctors track.
How Doctors Diagnose Brain Bleeds with Speed and Precision
Emergency physicians order non-contrast CT scans within minutes of arrival because these images reveal bright white blood collections against darker brain tissue and pinpoint exact location and size. MRI scans provide finer detail on surrounding edema and older bleeds when time allows, while CT angiography highlights active vessel leaks or aneurysms. Blood tests check coagulation status, platelet counts, and electrolyte balance to guide reversal agents and prevent further bleeding. Neurologists calculate Glasgow Coma Scale scores on the spot to gauge severity and predict immediate risks. Rapid diagnosis lets teams initiate life-saving measures before irreversible damage spreads.
Treatments That Improve Outcomes Every Day
Neurosurgeons remove large clots through minimally invasive techniques or open craniotomy when hematomas exceed safe volumes and cause dangerous shifts in brain structures. Intensivists lower elevated blood pressure with intravenous medications to stop ongoing bleeding without starving healthy tissue of perfusion. They reverse anticoagulants with specific agents like prothrombin complex concentrates or idarucizumab depending on the medication involved. Supportive care includes mechanical ventilation for comatose patients, seizure prevention, and careful fluid management to reduce swelling. Rehabilitation begins early with physical, occupational, and speech therapists who retrain affected functions and maximize independence.
Key Factors That Shape Recovery and Survival
Younger patients with smaller bleeds in non-critical areas and higher initial consciousness levels recover more function and return home sooner than older individuals with large deep hemorrhages. Prompt reversal of clotting problems and blood pressure control within the golden hour dramatically boost survival odds. Absence of intraventricular extension or herniation signs on imaging signals better prognosis because these complications multiply mortality risk. Comorbidities such as heart disease, diabetes, or prior strokes compound challenges, yet aggressive ICU management overcomes many obstacles. Genetic factors and overall fitness before the event also influence how well the brain rewires itself during recovery.
What are the chances of surviving a brain bleed when patients arrive at equipped stroke centers within the first hour? Modern protocols deliver survival rates that exceed historical figures through coordinated care bundles that include rapid imaging, blood pressure targets, and surgical readiness. Recent studies show 30-day survival for intracerebral hemorrhage reaches 50 to 70 percent in maximally treated cases, with five-year survival around 53 percent for those who receive full aggressive therapy. Location and volume still dominate outcomes, yet every advance in neurocritical care narrows the gap between life and loss.
What are the chances of surviving a brain bleed after doctors control the initial bleed and stabilize intracranial pressure? Patients with favorable Glasgow Coma Scale scores above 8 and hematomas under 30 milliliters often achieve independent living within months when they participate fully in rehabilitation. Ongoing research into minimally invasive clot removal and neuroprotective drugs continues to lift these percentages higher each year. Families who stay engaged and advocate for early therapy sessions see measurable gains in mobility, cognition, and quality of life that statistics alone cannot capture.
What are the chances of surviving a brain bleed for individuals on blood thinners who experience reversal within minutes of hospital arrival? Data confirm that ultra-rapid treatment cuts mortality significantly compared with delayed intervention, giving these patients a fighting chance even when initial scans look alarming. Multidisciplinary teams track every variable from admission labs to 24-hour imaging follow-ups to adjust plans dynamically. Survivors frequently credit this window of opportunity with preserving enough brain function for meaningful recovery.
Long-Term Recovery and Rehabilitation Strategies
Physical therapists mobilize patients as soon as swelling subsides and guide them through targeted exercises that rebuild strength and coordination lost to the bleed. Speech-language pathologists retrain swallowing safety and communication skills so survivors avoid aspiration pneumonia and reconnect with loved ones. Occupational therapists adapt daily living tools and home environments to restore independence in dressing, cooking, and personal care. Cognitive rehabilitation programs sharpen memory, attention, and problem-solving abilities that the bleed may have dulled. Support groups and psychological counseling address depression and anxiety that commonly follow such trauma and sustain motivation through the long haul.
Preventing Future Brain Bleeds Through Lifestyle and Medical Control
Physicians prescribe strict blood pressure regimens and monitor adherence because hypertension remains the top modifiable risk factor for recurrence. Patients quit smoking, limit alcohol, maintain healthy weight, and manage cholesterol and diabetes with proven medications and diet changes. Regular neurological check-ups catch new aneurysms or vascular malformations early through follow-up imaging when indicated. Doctors weigh risks and benefits of continuing or stopping anticoagulants after the acute phase and explore safer alternatives like left atrial appendage closure for certain heart conditions. Community education campaigns teach everyone to recognize stroke symptoms and call emergency services instantly.
What are the chances of surviving a brain bleed when prevention strategies combine with excellent acute care? Individuals who control underlying conditions and respond quickly to warning signs dramatically improve their personal odds and reduce population-wide burden. Public health initiatives that promote blood pressure screening and rapid transport to comprehensive stroke centers save thousands of lives annually. Ongoing global studies refine risk scores and personalize prevention plans so future generations face lower threats from this devastating condition.
What are the chances of surviving a brain bleed for those who experience recurrence after the first event? Annual recurrence risk hovers between 1 and 3 percent with optimal medical management, yet patients who maintain lifestyle changes and medication compliance lower this figure further. Long-term follow-up with vascular neurologists ensures early detection of new problems and timely adjustments to therapy. Survivors who embrace these measures often enjoy years of productive life after the initial crisis.
What are the chances of surviving a brain bleed compared with other stroke types when patients reach specialized centers? Hemorrhagic events carry higher short-term mortality than ischemic strokes, yet survivors frequently achieve comparable functional recovery through intensive rehabilitation. Advances in endovascular techniques for aneurysm securing and hematoma evacuation continue to close outcome gaps. Hope remains strong because research pipelines deliver new tools each year that translate directly into better survival and quality of life.
What are the chances of surviving a brain bleed in the era of personalized medicine and AI-assisted imaging? Algorithms now predict hematoma expansion risk within minutes of the first scan and guide surgeons to intervene precisely when benefit outweighs risk. Biomarker research identifies patients likely to benefit from experimental therapies and matches them to clinical trials rapidly. These innovations build on established protocols and push survival curves upward for even the most complex cases.
Conclusion: Knowledge Empowers Action
Brain bleeds test medical teams and families alike, yet rapid response, expert care, and dedicated rehabilitation turn many dire situations into stories of resilience. Patients who understand risk factors, recognize symptoms, and pursue evidence-based treatment position themselves for the best possible recovery. Communities that support stroke awareness and invest in specialized centers give every individual a stronger fighting chance.
While challenges persist, medical progress and human determination continue to improve outcomes and restore lives after this serious event. Consult healthcare professionals for personalized advice because timely action remains the most powerful ally in any brain bleed scenario.
READ ALSO: What Does a Torn ACL Feel Like: Symptoms, Causes, and Recovery

