Appendicitis strikes suddenly and demands immediate medical attention from healthcare professionals. Inflammation of the appendix triggers severe abdominal pain that often starts near the navel and shifts to the lower right side. Doctors perform emergency surgery in most cases to prevent rupture and life-threatening complications. Patients recover quickly when they seek treatment early, but delays lead to serious infections.
Lifestyle factors including diet influence the likelihood of developing this condition. Many individuals ask what food can cause appendicitis when they experience recurring digestive issues or family history concerns. Researchers examine dietary patterns closely because they identify preventable risk elements that millions overlook daily.
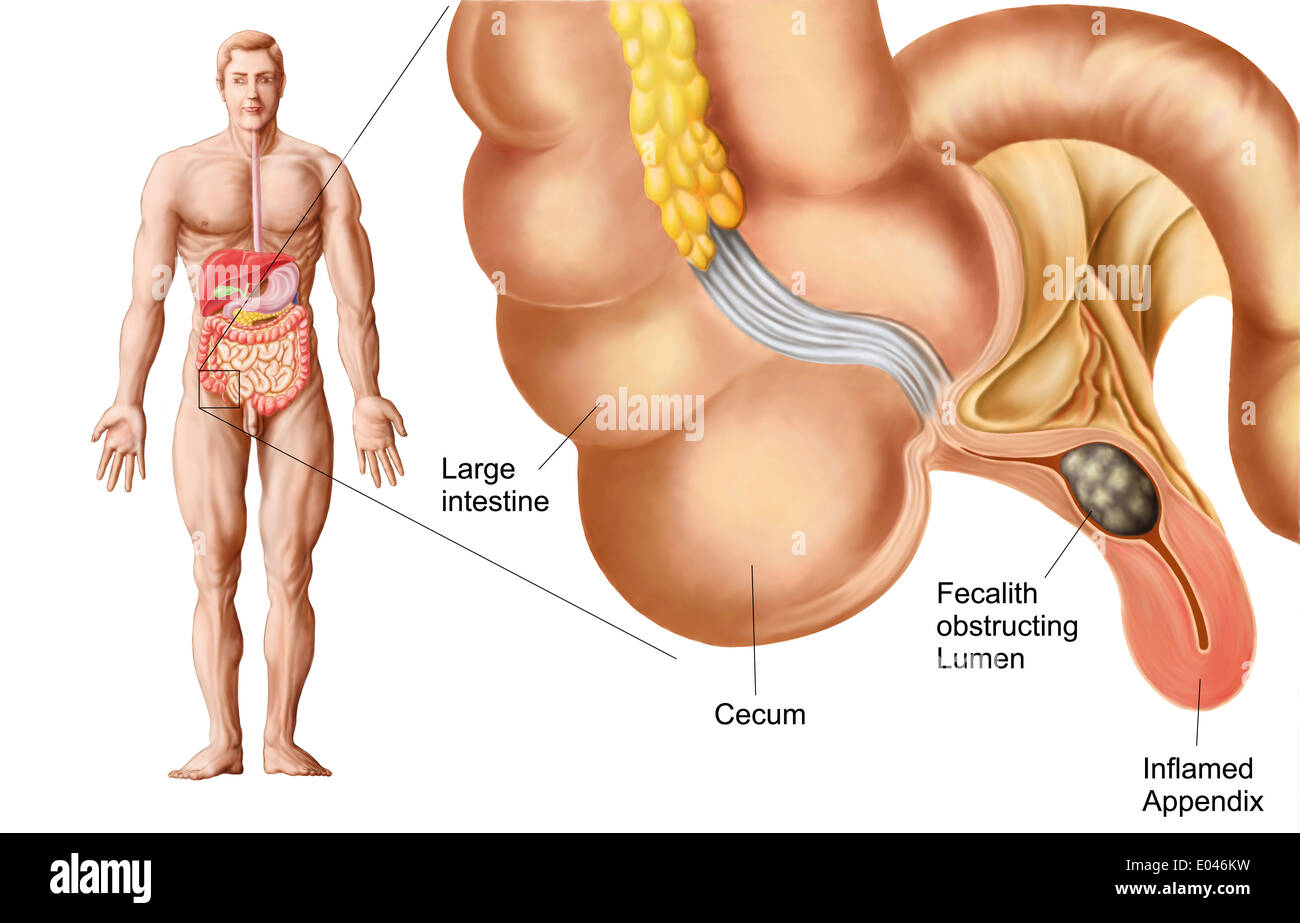
Understanding Appendicitis and Its Common Triggers
Doctors define appendicitis as inflammation of a small pouch attached to the large intestine. The appendix stores beneficial bacteria that support gut health during recovery from illnesses. Blockage in the appendix opening traps bacteria and leads to rapid swelling and pus formation. Infections from viruses or bacteria sometimes initiate the process without any dietary involvement. Trauma to the abdomen or tumors rarely contribute as well.
Individuals between ages 10 and 30 face the highest risk according to global health data. Men develop appendicitis slightly more often than women across populations. Early recognition of symptoms prevents complications that require extended hospital stays. Patients report nausea, vomiting, fever, and loss of appetite alongside the characteristic pain. Physicians use imaging tests like CT scans to confirm diagnosis before surgery. Prompt intervention saves lives and reduces recovery time dramatically.
The Dietary Connection to Appendicitis Risk
Nutrition experts connect eating habits directly to digestive system efficiency. Low-fiber diets slow intestinal movement and create hardened stool masses known as fecaliths. These masses block the appendix and promote bacterial overgrowth that sparks inflammation. High consumption of processed items reduces overall nutrient absorption and increases systemic inflammation. Scientists publish studies that link Western dietary patterns to elevated appendicitis rates worldwide.
People who maintain balanced meals experience fewer digestive blockages throughout their lives. Hydration supports fiber function by softening stool and preventing constipation episodes. Chronic low water intake compounds problems from poor food choices. Families pass down eating patterns that either protect or endanger appendix health across generations. Public health campaigns promote awareness because diet modifications offer simple prevention tools. Physicians advise patients to track daily fiber intake as part of routine wellness checks.
Foods That May Increase Your Appendicitis Risk
Processed meats and fried foods top the list of items that elevate digestive strain over time. Burgers, fries, and packaged snacks contain high levels of unhealthy fats that slow digestion dramatically. Red meat consumption in large quantities correlates with higher inflammation markers in multiple research reviews. Refined carbohydrates such as white bread and sugary pastries offer little bulk to keep bowels moving efficiently. Soft drinks and candy deliver empty calories that contribute to obesity and related complications.
Dairy products in excess create mucus that some individuals struggle to process smoothly. Spicy and acidic foods irritate the intestinal lining and worsen existing discomfort during flare-ups. Fast food meals combine multiple risk factors in single servings that people consume frequently. Cheese and butter add saturated fats that promote constipation when eaten regularly without balancing vegetables. Individuals who rely heavily on convenience foods face compounded risks from multiple sources simultaneously.
what food can cause appendicitis emerges as a frequent search term because people want practical guidance on daily choices. Healthcare providers explain that no single item triggers the condition instantly in healthy people. Cumulative effects from repeated poor decisions build pressure inside the digestive tract. Sugary snacks and refined grains reduce beneficial gut bacteria populations over months and years.
High-sodium items lead to fluid retention that affects overall abdominal comfort. People who eat these foods daily report more frequent constipation that sets the stage for blockages. Nutritionists recommend limiting these categories to occasional treats rather than staples. Restaurants serve oversized portions that encourage overconsumption of problematic ingredients. Home cooks who prepare fresh meals gain better control over ingredient quality and portion sizes. Awareness campaigns highlight these connections to empower informed shopping decisions at grocery stores.
Debunking Common Myths About Appendicitis and Food
Popular stories blame seeds and nuts for causing appendicitis through direct blockage. Medical literature shows these incidents occur in fewer than one percent of all cases examined. Popcorn kernels and fruit pits rarely lodge in the appendix according to large-scale surgical reviews. Individuals digest most seeds normally without any complications throughout their lifetimes. Guava seeds and similar small particles pass through the system harmlessly in the vast majority of eaters.
what food can cause appendicitis questions often stem from these persistent urban legends that doctors actively correct. Patients who chew food thoroughly eliminate even the minimal risks associated with hard particles. Studies of thousands of appendectomy specimens confirm fecaliths as the dominant cause rather than plant material. Parents sometimes restrict children’s diets unnecessarily based on outdated advice from previous generations. Modern gastroenterologists emphasize evidence-based information that frees people from unfounded fears while focusing on genuine prevention strategies.
High-Fiber Foods That Protect Against Appendicitis
Whole grains, fresh fruits, and vegetables form the foundation of an appendix-friendly eating plan. Oats, barley, and brown rice provide soluble fiber that softens stool and promotes regular bowel movements. Apples, pears, and berries deliver natural pectin that supports gut motility every day. Broccoli, carrots, and leafy greens add insoluble fiber that adds bulk and sweeps the intestines clean. Legumes such as lentils, chickpeas, and black beans offer protein alongside impressive fiber counts per serving.
Nuts and seeds in moderation supply healthy fats without the risks associated with overconsumption. People who consume 25 to 35 grams of fiber daily experience significantly lower appendicitis rates in population studies. Kiwis and prunes act as natural laxatives that maintain comfortable digestion without medication. Sweet potatoes and quinoa provide versatile options that fit easily into family meal rotations. Hydration amplifies fiber benefits by preventing the very blockages that lead to inflammation.

what food can cause appendicitis discussions always circle back to the protective power of fiber-rich choices. Nutritionists design meal plans that maximize variety while hitting daily targets consistently. Breakfast smoothies packed with spinach and berries deliver quick fiber boosts that sustain energy levels. Lunch salads loaded with mixed greens and beans create satisfying volumes without heavy calories.
Dinner stir-fries combine colorful vegetables with whole grains for complete nutrient profiles. Snacks of fresh fruit or vegetable sticks replace chips and maintain steady fiber intake between meals. Cooking methods matter because steaming preserves more fiber than over-processing does. Families that cook together develop lifelong habits that safeguard digestive health for decades. Supermarkets stock affordable high-fiber staples that fit every budget when shoppers plan ahead. Athletes and busy professionals benefit equally from these strategies that prevent unexpected medical emergencies.
Additional Lifestyle Factors That Complement Dietary Prevention
Regular physical activity stimulates intestinal contractions that move waste efficiently through the system. Walking after meals prevents sluggish digestion that contributes to fecalith formation over time. Stress management techniques reduce cortisol levels that otherwise slow gut function dramatically. Adequate sleep allows the digestive system to repair itself nightly without interference. Smoking and excessive alcohol intake damage intestinal linings and increase overall inflammation risks.
Maintaining a healthy body weight eliminates extra pressure on abdominal organs that complicates digestion. Probiotic-rich foods like yogurt and kefir support balanced gut bacteria that aid fiber processing. Annual check-ups allow doctors to monitor digestive patterns and suggest adjustments before problems escalate. Community programs teach these combined approaches because isolated diet changes produce limited results. Individuals who adopt comprehensive habits report fewer gastrointestinal complaints across all age groups.
Recognizing Symptoms and Seeking Timely Medical Care
Sudden sharp pain in the lower right abdomen signals the need for professional evaluation immediately. Loss of appetite and low-grade fever often accompany the discomfort that worsens with movement. Nausea and vomiting follow as inflammation progresses and irritates surrounding tissues. Rebound tenderness when doctors press and release the area confirms peritoneal involvement.
Blood tests reveal elevated white cell counts that indicate active infection. Ultrasound or CT imaging provides clear visualization of the swollen appendix before complications develop. Emergency rooms prioritize these cases because rupture risks rise rapidly within 24 to 48 hours. Parents notice children guarding their right side or walking bent forward during episodes. Adults sometimes mistake symptoms for gas or menstrual cramps until pain intensifies dramatically. Rapid response teams perform laparoscopic surgery that minimizes scarring and speeds recovery significantly.
Treatment Options and Post-Surgery Recovery Guidelines
Surgeons remove the inflamed appendix through small incisions in minimally invasive procedures that last under an hour. Antibiotics control infection before and after the operation in most standard cases. Patients resume light activity within days and return to normal routines within two weeks. Clear liquids progress to soft foods as bowel function returns under medical supervision. High-fiber meals resume gradually to avoid straining the healing incision site.
Pain management focuses on non-opioid options whenever possible to support natural recovery processes. Follow-up visits ensure complete healing and address any lingering digestive adjustments. Most individuals experience no long-term effects after successful appendectomy. Dietary counseling becomes part of discharge instructions because prevention remains key to avoiding other gut issues. Support groups connect patients who share experiences and tips for maintaining optimal digestive wellness afterward.
what food can cause appendicitis concerns fade once patients understand the bigger picture of prevention through consistent habits. Recovery programs reinforce the value of balanced nutrition that supports overall immune function. Families celebrate successful surgeries by adopting healthier collective eating patterns moving forward.
Research continues to explore genetic factors that interact with diet in determining individual susceptibility. Global health organizations promote fiber education because it delivers benefits far beyond appendix protection alone. Public awareness campaigns reach schools and workplaces to build lifelong knowledge about digestive health.
READ ALSO: How to Relieve Buttock Muscle Pain: Complete Guide for Fast Recovery

