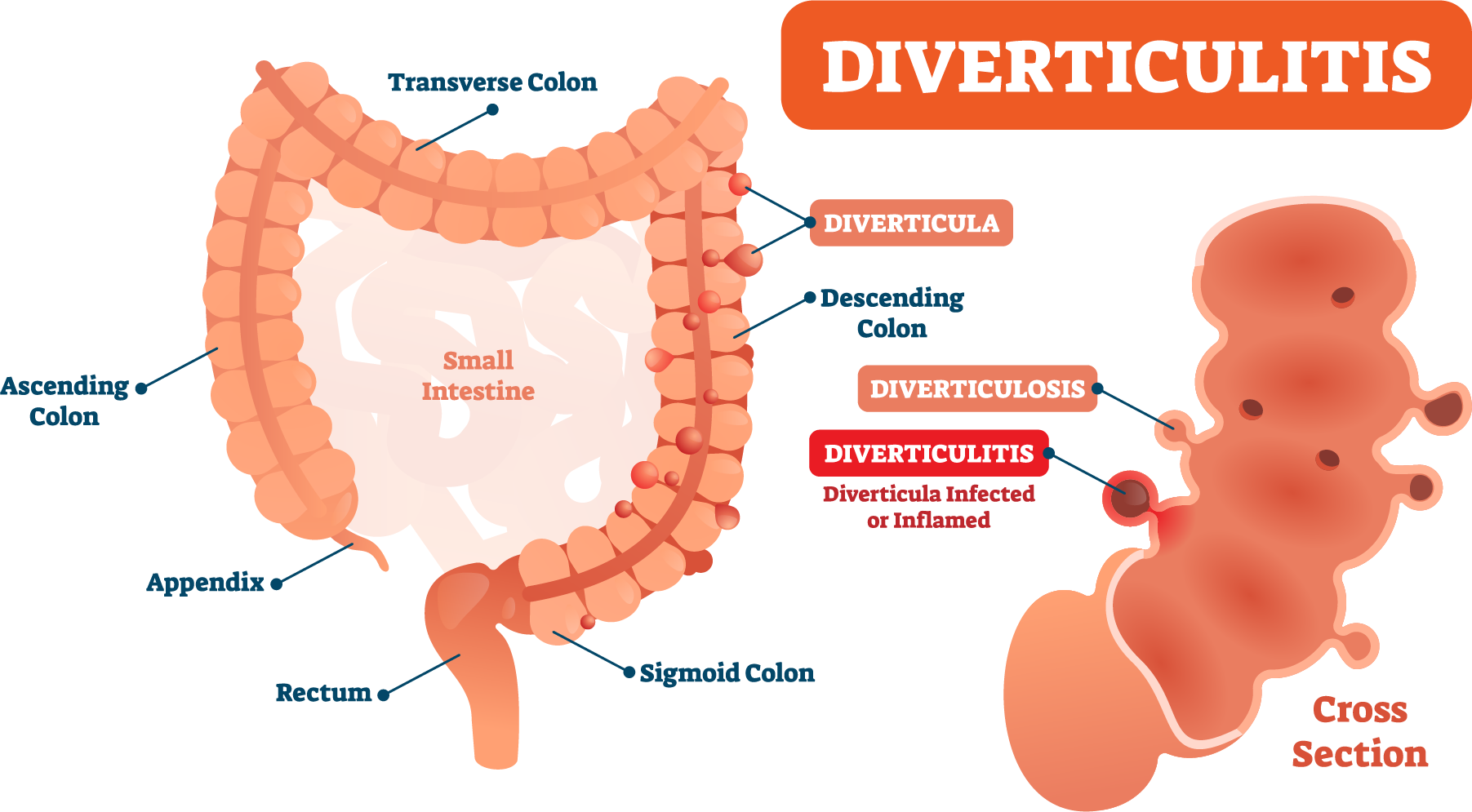
Introduction to Diverticulitis
Diverticulitis affects the digestive tract and causes inflammation in small pouches. These pouches form in the colon wall and are called diverticula. When these pouches become infected, the condition develops into diverticulitis. Many people manage mild cases with medication and diet changes. However, severe or recurring cases often require diverticulitis surgery.
Doctors recommend surgical treatment when complications arise. These complications include abscesses, perforations, or bowel obstruction. Understanding the procedure helps patients feel confident and prepared.
What Is Diverticulitis?
Diverticulitis develops when diverticula become inflamed or infected. These pouches usually form due to weak spots in the colon wall. Pressure from digestion pushes the lining outward and creates small sacs.
Symptoms vary depending on severity. Common symptoms include abdominal pain, fever, nausea, and changes in bowel habits. Pain usually occurs on the lower left side of the abdomen.
Doctors diagnose the condition using imaging tests like CT scans. Blood tests also help detect infection and inflammation.
When Is Surgery Necessary?
Doctors do not recommend surgery for every patient. Many cases improve with antibiotics and rest. However, certain situations require immediate medical intervention.
Severe Complications
Complications demand urgent surgical care. These include:
- Perforation of the colon
- Large abscess formation
- Fistulas between organs
- Intestinal blockage
In these cases, diverticulitis surgery becomes life-saving.
Recurrent Episodes
Frequent flare-ups weaken the colon over time. Repeated inflammation increases the risk of serious complications. Doctors often suggest surgery after multiple episodes.
Chronic Symptoms
Some patients experience ongoing discomfort and digestive problems. Surgery helps improve quality of life in such cases.
Types of Diverticulitis Surgery
Surgeons choose procedures based on the patient’s condition. They consider severity, overall health, and complications.
Primary Bowel Resection
This procedure removes the diseased portion of the colon. The surgeon reconnects the healthy ends afterward. This method allows normal bowel function to continue.
Many patients recover well after this type of diverticulitis surgery.
Bowel Resection with Colostomy
This procedure becomes necessary in emergency situations. The surgeon removes the infected section and creates an opening in the abdomen. Waste exits through a colostomy bag.
Doctors may reverse the colostomy later. This depends on healing and overall health.
Laparoscopic Surgery
Surgeons perform this minimally invasive procedure using small incisions. They use a camera and specialized tools to operate.
Patients experience less pain and faster recovery. Many prefer this modern approach when possible.
Open Surgery
Open surgery requires a larger incision in the abdomen. Surgeons use this method for severe infections or complications.
Recovery takes longer compared to laparoscopic techniques.
Preparing for Surgery
Preparation improves surgical outcomes and reduces risks. Doctors provide clear instructions before the procedure.
Medical Evaluation
Doctors review medical history and perform tests. These tests include blood work, imaging, and heart evaluations. They ensure the patient can handle surgery safely.
Diet Adjustments
Patients often follow a liquid diet before surgery. This step clears the digestive system and reduces complications.
Medication Management
Doctors may adjust medications before surgery. Patients stop certain drugs that increase bleeding risk.
Mental Preparation
Understanding the procedure reduces anxiety. Patients should discuss concerns with their healthcare provider.
The Surgical Procedure
Surgeons perform the operation under general anesthesia. The patient remains asleep and pain-free throughout the procedure.
The surgeon removes the affected portion of the colon. They then reconnect the healthy sections or create a colostomy if needed.
The duration depends on complexity. Most procedures take several hours.
Risks and Complications
Every surgery carries risks. Patients should understand possible complications before undergoing diverticulitis surgery.
Common Risks
- Infection at the surgical site
- Bleeding during or after surgery
- Blood clots
- Reactions to anesthesia
Specific Complications
- Leakage at the reconnection site
- Injury to nearby organs
- Prolonged bowel inactivity
Doctors monitor patients closely to prevent complications.
Recovery After Surgery
Recovery varies based on the type of procedure and patient health. Proper care speeds up healing and reduces risks.
Hospital Stay
Patients usually stay in the hospital for several days. Doctors monitor vital signs and bowel function during this period.
Pain Management
Doctors provide medications to control pain. Managing pain helps patients move and recover faster.
Diet Progression
Patients start with liquids after surgery. They gradually move to soft and then solid foods.
Physical Activity
Light movement helps prevent blood clots and improves circulation. Patients should avoid heavy lifting during recovery.
Long-Term Lifestyle Changes
Lifestyle changes play a crucial role after diverticulitis surgery. These changes help prevent recurrence and improve overall health.
High-Fiber Diet
Fiber supports healthy digestion and reduces pressure in the colon. Foods like fruits, vegetables, and whole grains help maintain bowel health.
Hydration
Drinking enough water supports digestion and prevents constipation. Patients should maintain consistent hydration daily.
Regular Exercise
Physical activity improves digestive function and overall well-being. Even light exercise offers significant benefits.
Avoiding Smoking
Smoking slows healing and increases complications. Quitting smoking improves long-term outcomes.
Diet Tips After Surgery
Diet plays a major role in recovery and prevention. Patients should follow medical advice carefully.
Early Recovery Diet
- Clear broths
- Gelatin
- Water and electrolyte drinks
Transition Foods
- Mashed potatoes
- Soft fruits
- Cooked vegetables
Long-Term Diet
Patients should adopt a balanced, high-fiber diet. They should avoid processed foods and excessive red meat.
Emotional and Psychological Impact
Surgery affects both physical and mental health. Patients may feel anxious or stressed during recovery.
Support from family and friends improves emotional well-being. Counseling also helps patients cope with changes.
Maintaining a positive outlook supports faster recovery and better health outcomes.
Cost and Accessibility
The cost of surgery varies based on location and hospital facilities. Insurance often covers medically necessary procedures.
Patients should discuss costs and coverage with their healthcare provider. Understanding expenses prevents financial stress.
Preventing Future Episodes
Prevention reduces the need for additional medical treatment. Patients should follow healthy habits consistently.
Healthy Eating
A fiber-rich diet keeps the digestive system functioning properly.
Regular Checkups
Routine medical visits help detect early signs of complications.
Stress Management
Stress affects digestion and overall health. Relaxation techniques improve well-being.
Benefits of Surgery
Surgery offers long-term relief for severe cases. It removes the diseased portion of the colon and prevents complications.
Patients often experience improved quality of life. Pain decreases, and normal digestion resumes.
For many individuals, diverticulitis surgery provides a permanent solution.
Who Is a Good Candidate?
Not every patient requires surgery. Doctors evaluate each case carefully.
Ideal candidates include:
- Patients with repeated infections
- Individuals with complications
- Patients with poor response to medication
Doctors assess overall health before recommending surgery.
Advances in Surgical Techniques
Modern medicine continues to improve surgical outcomes. Minimally invasive techniques reduce recovery time and pain.
Robotic-assisted surgery offers greater precision. These advancements make procedures safer and more effective.
Patients benefit from shorter hospital stays and faster healing.
Frequently Asked Questions
Is Surgery Painful?
Patients do not feel pain during surgery due to anesthesia. Pain after surgery is manageable with medication.
How Long Does Recovery Take?
Recovery usually takes several weeks. Full recovery depends on the procedure and individual health.
Can Diverticulitis Return After Surgery?
Surgery reduces the risk significantly. However, healthy lifestyle choices remain important.
Final Thoughts
Diverticulitis can disrupt daily life and cause serious health issues. Early treatment helps manage mild cases effectively. However, severe conditions often require medical intervention.
Understanding the process helps patients make informed decisions. Diverticulitis surgery offers relief from recurring pain and complications. With proper care, most patients return to normal life. Maintaining a healthy lifestyle remains essential after treatment. A balanced diet, regular exercise, and medical follow-ups ensure long-term success.
READ ALSO: How to Get Phlegm Out of Chest: Complete Relief Guide