Eye care professionals stress that anyone who notices changes in their vision must understand detached retina symptoms to avoid irreversible harm. The retina serves as the crucial film that captures light and converts it into signals the brain interprets as sight. When detachment occurs, patients lose the ability to process images from the affected area. Immediate recognition allows doctors to reattach the tissue before permanent blindness sets in. This comprehensive guide examines every facet of the condition, equipping readers with the knowledge they need to protect their eyesight effectively.
What Is Retinal Detachment and Why Does It Happen
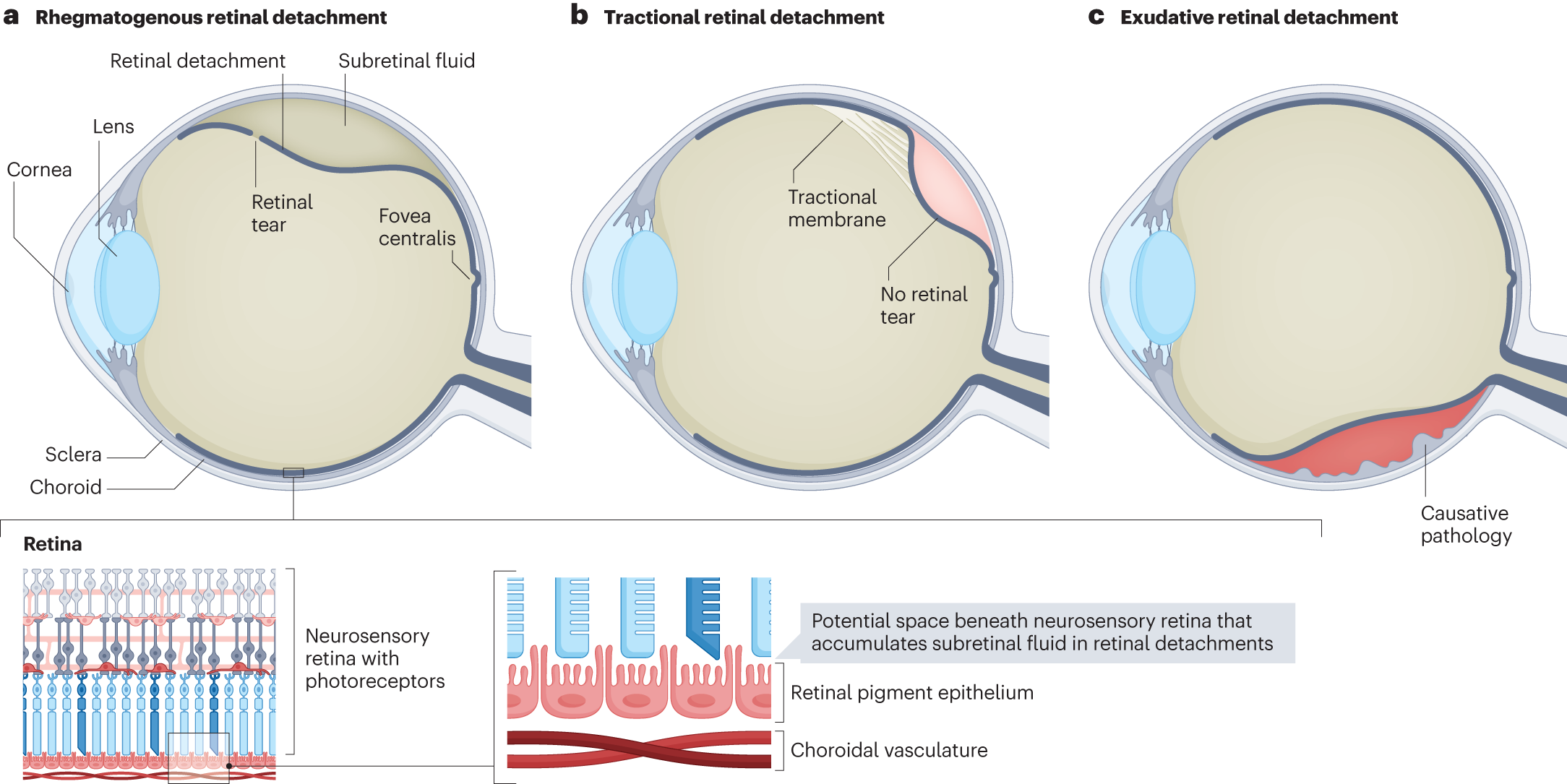
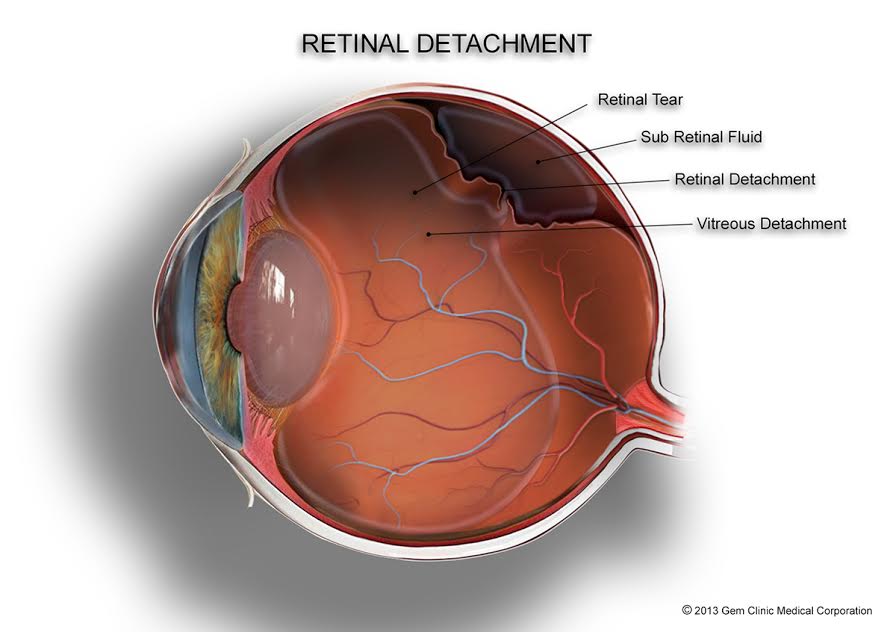
The retina functions as the light-sensitive layer at the back of the eyeball. It sends visual information through the optic nerve to the brain. When the retina detaches, it separates from the supportive tissue and loses its blood supply. Oxygen and nutrients no longer reach the cells, and vision fades rapidly. Surgeons classify the condition into rhegmatogenous, tractional, and exudative varieties based on the mechanism. Rhegmatogenous detachment develops when a tear allows fluid to flow underneath. Tractional forms arise from scar tissue pulling the retina away. Exudative types result from fluid leakage due to inflammation or tumors without any tear.
The vitreous humor, the clear gel filling the eye chamber, maintains pressure and shape throughout life. As individuals age, this gel contracts and separates from the retina in a process called posterior vitreous detachment. Most people experience only mild floaters during this phase, but in some cases the separation rips the delicate retinal tissue.
Fluid rushes through the tear and lifts the retina like a blister. Without prompt repair, the detached section starves for nutrients and dies. High levels of myopia elongate the eyeball and increase tension on the retina. Cataract surgery or prior eye injuries also weaken structural supports. Diabetic retinopathy promotes fibrous bands that tug relentlessly. These mechanisms explain why certain populations face elevated risks and why regular monitoring proves essential.
Doctors perform thorough examinations to confirm detachment and determine the type. Ultrasound imaging reveals hidden tears when the view inside the eye remains obscured. Optical coherence tomography provides detailed cross-sections that guide surgical planning. Patients benefit from early diagnosis because the macula, the central vision area, stays functional longer. Once the macula detaches, recovery prospects diminish sharply. Eye surgeons emphasize regular checkups for at-risk groups because prevention beats treatment every time.
Risk Factors That Increase Your Chances
Age represents the primary risk factor because vitreous changes accelerate after 50. Nearsighted people possess longer eyeballs that stretch retinal tissue thin and prone to tears. Family members who experienced detachment pass along genetic predispositions that weaken attachments. Previous eye surgeries introduce scar tissue that contracts over time.
Trauma from sports or accidents delivers blunt force that shakes the vitreous violently. Chronic conditions like diabetes damage retinal blood vessels and encourage proliferative growth. Inflammatory diseases such as uveitis leak fluid that accumulates underneath the retina. Individuals who ignore these risks often discover problems too late.
Lifestyle choices including smoking impair vascular health and slow healing. Maintaining stable blood sugar and blood pressure protects the delicate structures inside the eye. Athletes in contact sports wear protective eyewear to minimize blunt trauma.
People with a history of eye surgery attend follow-up visits religiously. These proactive steps dramatically reduce the likelihood of detachment and preserve lifelong vision quality. Communities in regions with high diabetes prevalence benefit from targeted education programs that highlight these connections.
Common detached retina symptoms Everyone Should Know
Patients monitor their vision closely and catch changes before extensive damage develops. Sudden showers of new floaters appear as black specks or cobwebs drifting across the field of view. These floaters result from debris in the vitreous casting shadows on the retina. Bright flashes of light, known as photopsia, occur when the vitreous tugs on retinal nerves. The flashes resemble lightning or camera bulbs and happen even in darkened rooms.
A dark shadow or curtain sweeps across the peripheral vision from one side. This shadow signals advancing detachment that blocks light from reaching the retina. Blurred central vision follows if the macula becomes involved. Patients lose the ability to read fine print or recognize faces. Straight lines appear wavy or distorted in early stages. Color perception fades in the affected region. These changes progress rapidly within hours or days.

Ophthalmologists advise patients to cover one eye at a time and test each separately because detachment often affects only one eye initially. Sudden onset distinguishes these signs from gradual age-related changes. Migraine auras produce similar flashes but resolve quickly whereas retinal issues persist and worsen.
Floaters from normal aging increase slowly while detachment brings hundreds at once. Patients who experience detached retina symptoms should not drive or operate machinery until evaluated by a specialist. Emergency rooms equipped with eye specialists evaluate and treat within hours when necessary. Timely action prevents the curtain effect from advancing further and safeguards remaining vision.
Advanced Signs That Demand Emergency Care
When changes advance unchecked, patients notice a large veil blocking half their visual field. The curtain effect starts peripherally and moves centrally as more retina lifts away. Complete vision loss in one eye occurs if the entire retina separates. Pain remains absent because the retina lacks pain receptors, which lulls some people into false security.
Bilateral involvement happens rarely but requires even faster response. Secondary complications like vitreous hemorrhage cloud the view further with blood. Macular involvement destroys sharp central vision permanently if untreated beyond 24 hours. Surgeons achieve 90 percent reattachment success when they intervene early, but rates drop once the macula detaches. Patients who report these advanced signs receive priority scheduling for operating rooms.
Diagnosis Methods Eye Doctors Use
Ophthalmologists dilate the pupils with drops to examine the retina directly using special lenses. Indirect ophthalmoscopy allows viewing the peripheral retina where tears often hide. Slit-lamp biomicroscopy provides magnified views of the front and back structures. B-scan ultrasonography generates images when dense cataracts or hemorrhage obscure the view.
Optical coherence tomography scans produce high-resolution layers that pinpoint fluid pockets. Fluorescein angiography highlights leaking vessels associated with exudative types. These tests confirm the diagnosis and map the extent of detachment for surgical strategy. Patients undergo these procedures comfortably in office settings within minutes. Results guide whether laser, gas bubble, or vitrectomy offers the best repair option.
Treatment Options Available Today
Surgeons select procedures based on detachment size, location, and patient health. Pneumatic retinopexy involves injecting a gas bubble that presses the retina back into place while laser seals the tear. The patient maintains a specific head position for days to keep the bubble in contact. Scleral buckling places a silicone band around the eye to relieve vitreous traction and support the retina externally.
Vitrectomy removes the vitreous gel entirely and replaces it with saline or oil while applying laser or cryotherapy to seal breaks. Each technique restores anatomy and prevents further fluid accumulation. Success rates exceed 85 percent overall, with multiple procedures sometimes necessary for complex cases. Patients receive local or general anesthesia depending on the approach. Post-operative care includes antibiotic drops, anti-inflammatory medications, and activity restrictions to promote healing.
Research continues to refine these methods with smaller instruments and faster recovery protocols. Minimally invasive options reduce scarring and improve cosmetic outcomes. Surgeons combine techniques when single procedures prove insufficient. Patients discuss all options thoroughly with their retinal specialist to choose the approach that best fits their lifestyle and medical history.
Recovery Process and What to Expect
Patients leave the hospital the same day or after overnight observation following most procedures. Gas bubbles dissolve naturally over weeks while silicone oil requires later removal surgery. Positioning requirements test patience but determine success. Vision improves gradually as swelling subsides and the retina reattaches firmly.
Full recovery takes three to six months depending on macular involvement. Cataract formation represents a common side effect of vitrectomy that surgeons address later. Regular follow-up visits monitor for redetachment or new tears in the fellow eye. Most patients regain functional vision sufficient for daily activities even if perfect clarity never returns. Support groups connect individuals facing similar journeys and share coping strategies. Families learn to recognize warning signs so they assist loved ones promptly.
Prevention Strategies That Work
Regular comprehensive eye exams detect early tears before they progress to full detachment. Optometrists dilate pupils and inspect the periphery during routine visits. High-risk individuals schedule checks every six months instead of annually. Protective eyewear prevents trauma during sports or hazardous work.
Controlling diabetes and hypertension preserves retinal blood flow. Smoking cessation improves vascular health throughout the body including the eyes. Patients who undergo cataract surgery follow post-operative instructions precisely to minimize complications. Awareness campaigns educate communities about sudden visual changes that warrant immediate evaluation. Simple lifestyle adjustments dramatically lower incidence rates in vulnerable populations. Parents teach children the importance of eye safety from a young age.
The Importance of Immediate Medical Attention
Patients who recognize detached retina symptoms and contact specialists immediately experience superior recovery rates. Delays beyond 48 hours increase the likelihood of proliferative vitreoretinopathy, a scarring complication that complicates repair. Emergency departments triage eye complaints based on symptom severity.
Telemedicine consultations sometimes bridge the gap until in-person evaluation. Transportation arrangements ensure patients reach facilities equipped for retinal surgery. Community awareness programs teach first responders to identify visual emergencies. These coordinated efforts save countless eyes from permanent impairment and reduce healthcare costs associated with long-term vision loss.
Myths and Facts About Retinal Detachment
Many believe detached retina symptoms always involve pain, yet the condition remains painless throughout. Others assume only elderly people face risk, but young athletes sustain traumatic detachments regularly. Some delay treatment thinking floaters resolve naturally, but detachment-related ones signal danger.
Correct information dispels these misconceptions and encourages proactive behavior. Reliable sources from ophthalmology associations provide accurate guidance. Patients who verify facts avoid unnecessary panic or dangerous complacency. Sharing accurate knowledge within families strengthens collective eye health vigilance.
Future Advances in Treatment and Prevention
Researchers develop new biomaterials for better buckling and tamponade agents that dissolve faster. Gene therapies target hereditary weaknesses that predispose families to detachment. Artificial intelligence analyzes retinal scans to predict detachment risk years in advance. Minimally invasive techniques reduce recovery time and complications. Public health initiatives promote widespread screening in aging populations. These innovations promise to lower incidence and improve outcomes globally while making treatments accessible even in remote areas.
Conclusion: Take Control of Your Eye Health Today
Understanding detached retina symptoms empowers individuals to safeguard their most precious sense. Regular checkups combined with prompt response to changes create the best defense. Families discuss vision health openly and support one another in seeking care. Communities benefit when everyone recognizes the urgency of these symptoms. By staying informed and vigilant, people preserve clear vision for decades of active living. Schedule an eye exam this month and share this knowledge with loved ones to create a ripple effect of awareness and prevention.
READ ALSO: How to Fix Hammer Toe: Complete Guide for Fast Relief