Introduction of Occipital Nerve Block
Patients battling chronic headaches often feel trapped in a cycle of pain that steals their productivity and joy. Medical experts now offer targeted solutions that deliver rapid results without major surgery. This comprehensive guide explores every aspect of modern headache management through precise nerve interventions, empowering readers to make informed decisions about their health. Readers discover how specialists pinpoint pain sources, perform quick outpatient procedures, and help individuals reclaim active lifestyles filled with energy and focus.

Understanding the Anatomy of Headache Triggers
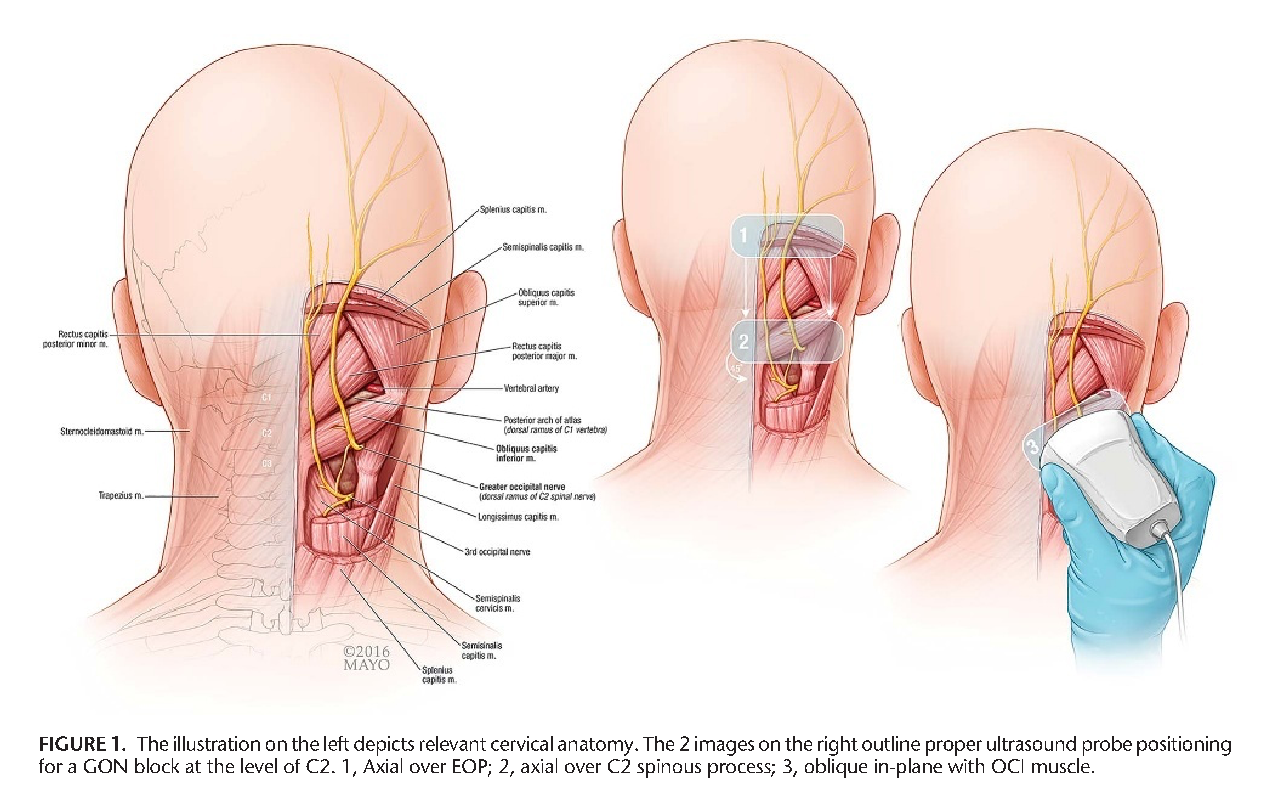
Nerves in the upper neck and back of the head transmit signals that control sensation across the scalp and forehead. The greater and lesser occipital nerves branch from the cervical spine and weave through muscles before reaching the skin surface. Inflammation or compression in these pathways creates intense, throbbing discomfort that radiates from the base of the skull to the eyes.
Physicians map these exact routes using advanced imaging to ensure treatments address root causes rather than symptoms alone. Knowledge of this neural network allows doctors to interrupt faulty signals at their origin and restore normal function quickly. Patients who learn the anatomy behind their pain gain confidence in pursuing effective care that targets specific trigger points rather than relying on temporary medications.
Conditions That Respond Well to Targeted Nerve Interventions
Occipital neuralgia strikes when irritated nerves fire constant pain messages, mimicking migraine attacks but originating from the neck. Cluster headaches cluster in predictable patterns and respond dramatically when specialists calm overactive pathways. Post-traumatic head injuries often leave lingering nerve sensitivity that escalates with movement or light touch.
Cervicogenic headaches stem from neck joint problems yet manifest as severe head pain that disrupts sleep and concentration. Migraine sufferers with occipital involvement experience fewer attacks after precise treatment calms the nerves. Doctors evaluate medical history, perform physical exams, and review imaging studies to confirm the nerve as the primary culprit before recommending intervention.
How Specialists Perform the Procedure with Precision
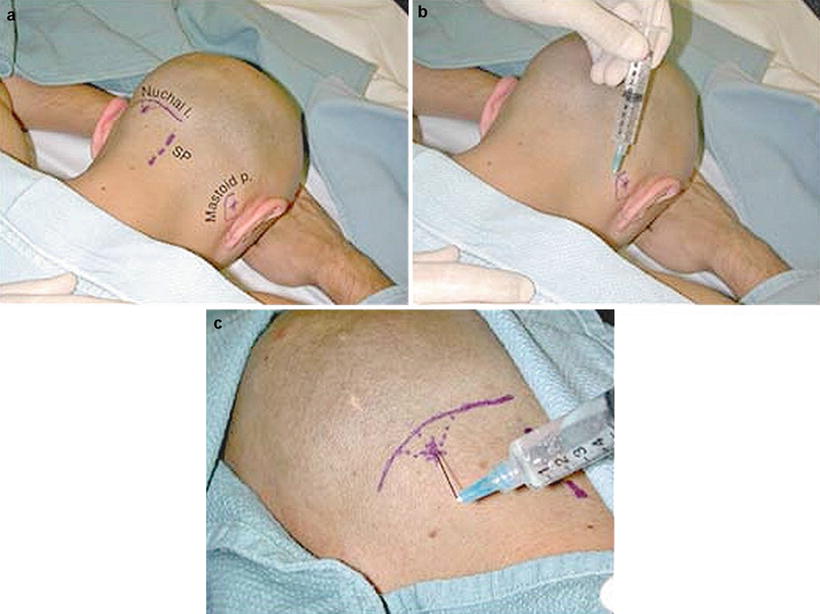
Physicians position patients comfortably on their stomach or side in a sterile outpatient setting. They clean the skin at the base of the skull and apply local anesthetic to minimize discomfort during the process. Using anatomical landmarks or ultrasound guidance, doctors locate the exact nerve exit points near the occipital ridge.
They then inject a mixture of long-acting anesthetic and anti-inflammatory medication directly around the nerve sheath. The entire process takes less than fifteen minutes, and patients remain awake to report sensations that help confirm accurate placement. Specialists monitor vital signs throughout to ensure safety while delivering immediate pain-blocking effects that last hours to months depending on the individual response.
Medical teams adjust medication concentrations based on patient tolerance and pain severity to optimize outcomes. Ultrasound guidance improves accuracy and reduces risks compared to landmark techniques alone. Patients feel a brief pressure sensation during injection followed by warmth as the medication spreads along the nerve. Doctors encourage gentle neck movements post-procedure to distribute the solution evenly and enhance relief duration. This minimally invasive approach avoids general anesthesia and allows individuals to resume normal activities the same day in most cases.
Immediate and Long-Term Benefits Patients Experience
Individuals report sharp reductions in headache intensity within minutes of treatment completion. Daily activities become enjoyable again as pain no longer dictates schedules or limits social interactions. Many reduce or eliminate reliance on strong pain medications that cause side effects like drowsiness or stomach issues.
Improved sleep quality follows because nighttime headaches no longer interrupt rest cycles. Patients return to work, exercise routines, and family responsibilities with renewed vigor and mental clarity. Long-term studies show sustained relief for six to twelve months in a majority of cases, with repeat procedures extending benefits further. Enhanced quality of life scores reflect better mood, concentration, and overall well-being after successful interventions.
Preparation Steps That Ensure Optimal Results
Doctors instruct patients to stop blood-thinning medications several days before the appointment to minimize bruising risks. Individuals fast for a few hours if sedation is planned, though most procedures require no sedation. Patients arrange transportation home because mild numbness in the scalp can affect coordination temporarily.
Specialists review allergies and current health conditions to select the safest medication combination. Pre-procedure consultations include detailed discussions about expected sensations and realistic outcome timelines. Hydration and light meals help patients feel comfortable during the short visit. Clear communication between patient and doctor builds trust and contributes to higher satisfaction rates.
What Happens During Recovery and Follow-Up Care
Patients rest briefly in the clinic while nurses monitor for any immediate reactions. Mild soreness at the injection site typically fades within twenty-four hours. Ice packs applied for ten minutes several times daily reduce swelling and promote comfort. Doctors advise avoiding strenuous neck exercises for forty-eight hours to allow the medication to settle.
Most individuals drive themselves home and return to work the next day. Follow-up appointments at two weeks assess pain levels and determine if additional treatments would provide further benefits. Specialists track progress through pain diaries that patients maintain to identify patterns and refine future care plans. Consistent communication ensures adjustments happen quickly when needed.
Potential Risks and How Experts Minimize Them
Skilled practitioners use sterile techniques and precise needle placement to keep complication rates extremely low. Temporary numbness or tingling in the scalp occurs in some cases but resolves within days. Infection risks remain minimal when clinics follow strict protocols.
Allergic reactions to medications happen rarely and receive immediate attention in the facility. Bleeding or hematoma formation stays uncommon because doctors screen for clotting issues beforehand. Patients receive clear instructions about warning signs that warrant prompt medical contact. Experienced providers discuss every possible outcome transparently so individuals make fully informed choices about proceeding with care.
Success Rates Backed by Clinical Observations
Large patient cohorts demonstrate that seventy to eighty percent of individuals achieve meaningful pain reduction after the first treatment. Repeat procedures often build on initial success and extend relief periods significantly. Factors like early intervention, accurate diagnosis, and proper technique influence outcomes positively.
Younger patients and those without extensive prior surgeries tend to respond especially well. Specialists combine the intervention with physical therapy or posture correction to amplify and prolong benefits. Real-world data from headache clinics worldwide confirm high patient satisfaction and improved daily functioning scores post-treatment. Ongoing research refines techniques and expands applications to additional pain conditions.
Comparing Options: When This Approach Outperforms Others
Oral medications provide temporary relief yet often lose effectiveness over time and carry systemic side effects. Physical therapy strengthens supporting muscles but may not calm irritated nerves quickly enough for severe cases. Botox injections target different pathways and require frequent office visits. Surgical decompression offers permanent solutions for select patients but involves longer recovery.
The targeted nerve approach sits comfortably between conservative and invasive options, delivering fast results with minimal downtime. Patients who failed multiple prior treatments frequently find success here because it directly addresses the nerve source rather than masking symptoms. Doctors collaborate with multidisciplinary teams to create personalized plans that combine the best elements of available therapies.
Lifestyle Changes That Enhance Treatment Effectiveness
Regular neck stretches and strengthening exercises maintain proper alignment and reduce nerve compression between procedures. Stress management techniques like meditation lower overall muscle tension that exacerbates headaches. Consistent sleep schedules support nervous system recovery and prevent flare-ups. Hydration and balanced nutrition supply essential nutrients that keep nerves healthy.
Ergonomic workstations prevent forward head posture that strains cervical structures. Patients who adopt these habits report fewer recurrences and longer intervals between interventions. Support groups connect individuals with others who share similar experiences and practical coping strategies. Holistic approaches complement medical procedures and create comprehensive pain management ecosystems.
Who Should Consult a Specialist for Evaluation
Persistent headaches that last more than four hours several times weekly signal the need for professional assessment. Pain localized to the back of the head with tenderness on palpation points toward nerve involvement. Associated symptoms like light sensitivity, nausea, or visual changes warrant thorough investigation.
Individuals whose headaches worsen with neck movement benefit from specialized evaluation. Those who have tried multiple medications without lasting success find new hope through expert consultation. Primary care doctors refer appropriate candidates to pain management or neurology specialists who perform detailed assessments. Early evaluation prevents chronic pain patterns from becoming entrenched and improves long-term prognosis.
Advanced Techniques That Improve Accuracy and Comfort
Ultrasound guidance allows real-time visualization of nerves and blood vessels during injection. Fluoroscopy provides additional confirmation in complex anatomy cases. Platelet-rich plasma injections offer regenerative options for patients seeking longer-lasting natural relief. Radiofrequency ablation extends benefits by creating controlled heat lesions that disrupt pain signals for extended periods.
Specialists select techniques based on individual anatomy and response history to maximize success. Training programs ensure providers master the latest innovations before implementing them in clinical practice. Continuous education keeps techniques at the forefront of pain management science.
Building a Supportive Care Team for Lasting Success
Neurologists, pain specialists, physical therapists, and psychologists collaborate to address every dimension of chronic headache disorders. Coordinated care plans prevent gaps that allow pain to return. Regular team meetings review progress and adjust strategies promptly. Patients receive education about their condition that empowers active participation in recovery.
Family members learn supportive roles that reduce household stress during treatment phases. Community resources provide additional layers of encouragement and practical assistance. Integrated care models consistently outperform fragmented approaches in patient-reported outcomes and quality-of-life metrics.
Future Developments in Nerve Pain Management
Researchers explore longer-acting medications that extend relief beyond current durations. Regenerative therapies using stem cells show promise in repairing damaged nerve tissues. Wearable devices that monitor nerve activity help predict and prevent flare-ups before they intensify. Personalized medicine approaches analyze genetic factors to customize medication selections.
Minimally invasive implants may one day offer on-demand nerve modulation without repeated injections. Clinical trials continue to expand understanding of headache mechanisms and refine intervention protocols. Patients who stay informed about emerging options position themselves to benefit from breakthroughs as they become available.
Taking the Next Step Toward Pain-Free Living
Knowledge transforms uncertainty into confidence when facing chronic pain challenges. Individuals who understand their options approach consultations prepared and engaged. Specialists welcome questions and provide detailed explanations tailored to each unique situation. Scheduling an evaluation opens doors to personalized plans that fit busy lifestyles and specific health needs. Supportive environments help patients navigate the journey from pain to relief with dignity and optimism. Every success story begins with a single decision to seek expert guidance and explore proven solutions.
This guide equips readers with actionable information that drives better health decisions. Readers who apply these insights often experience dramatic improvements in daily comfort and overall well-being. Medical advancements continue to evolve, yet the core principle remains constant: precise targeting of pain sources delivers superior results. Individuals ready to break free from headache limitations find powerful allies in modern nerve interventions that restore freedom and vitality.
READ ALSO: What does a Bunion look like and How It Appears on Feet