Foot pain can limit movement, reduce comfort, and affect daily routines. Many people ignore mild pain until walking becomes difficult. One common cause is a bone spur on top of foot. This condition often develops slowly and worsens with pressure, tight shoes, or repeated strain. Early awareness helps prevent long-term discomfort and mobility issues.
A bone spur is a small bony growth that forms along the edge of a bone. It usually appears where joints experience stress or where tendons pull repeatedly. While some bone spurs cause no symptoms, others create pain, swelling, and shoe irritation. Understanding why they form and how to treat them can help restore comfort and movement.
Doctors trace most cases to osteoarthritis where cartilage between foot bones wears down gradually. The body responds by generating extra bone along joint edges to distribute pressure. Repetitive impact from running or jumping accelerates this process in the midfoot region. Tight shoes that rub against the dorsum create constant friction and trigger inflammation. Abnormal foot mechanics such as high arches or flat feet add uneven stress that promotes growth. Trauma from sprains or fractures also initiates spur formation as healing tissue overcompensates. Genetic factors influence susceptibility in some families where joint degeneration runs strong.
What Triggers These Dorsal Foot Projections
Healthcare professionals identify several key factors that contribute to bony overgrowths in the upper foot area. Osteoarthritis stands out as the primary driver because it erodes protective cartilage layers. Without adequate cushioning bones rub together and prompt the body to form stabilizing spurs. Athletes who engage in high-impact sports expose their midfoot joints to repeated microtrauma. This cumulative damage encourages osteophyte development over months or years. Improper footwear plays a major role too. Shoes lacking sufficient toe box width or arch support compress soft tissues against bone surfaces.
Foot structure abnormalities amplify risk significantly. Individuals with high arches experience greater pressure on the top during gait cycles. Flat feet distribute weight unevenly and strain ligaments that attach to tarsal bones. Previous injuries like ankle sprains leave scar tissue that alters biomechanics. The altered motion pattern then stresses dorsal joints and invites spur growth. Age-related changes reduce joint flexibility and make older adults more vulnerable. Excess body weight increases load on every step and heightens inflammation potential. Researchers link these elements to higher incidence rates in active populations.
A bone spur on top of foot frequently connects to midfoot arthritis patterns that specialists observe in clinical settings. Patients who ignore early warning signs often report worsening symptoms during prolonged standing. Preventive measures focus on addressing these root causes before growths become problematic. Regular foot assessments help catch biomechanical issues early. Orthopedic experts recommend custom evaluations for anyone with family history of joint conditions.
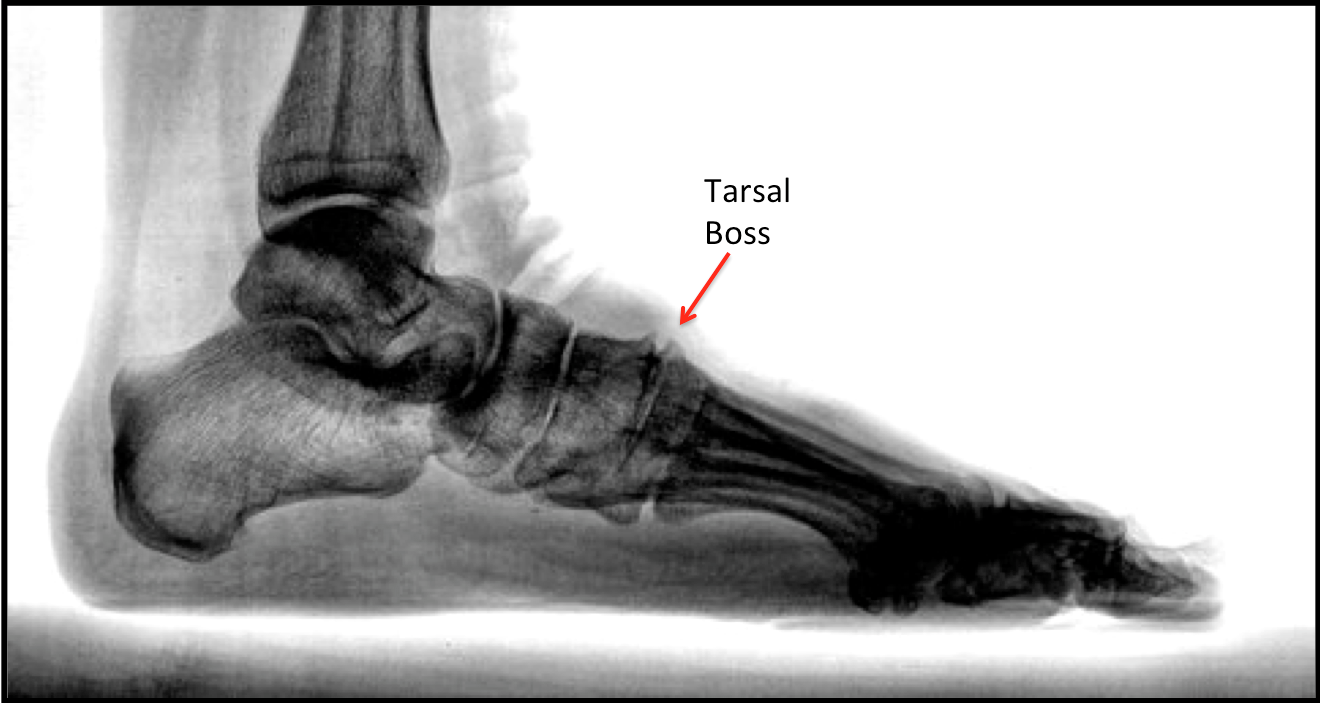
Identifying Common Symptoms of Upper Foot Bone Projections
Patients report sharp or aching sensations along the top of the foot that intensify with movement. Swelling and redness appear around the affected joint as inflammation builds. Stiffness limits normal range of motion especially after periods of rest. Many individuals struggle to wear closed shoes because the bony bump presses against the material. Tenderness develops when pressure applies directly over the growth. Limited joint mobility affects balance and gait patterns over time.
Advanced cases produce visible lumps that feel firm to the touch. Pain radiates toward the toes or ankle during weight-bearing activities. Some experience burning sensations if nerves become irritated nearby. Morning discomfort often peaks because overnight stiffness combines with initial steps. Athletes notice performance drops as the condition restricts push-off power. Daily tasks like climbing stairs become challenging when inflammation flares. Early symptom recognition allows prompt intervention and avoids complications like secondary tendon strain.
How Specialists Confirm the Presence of These Growths
Podiatrists begin evaluations with thorough physical examinations that assess tenderness and range of motion. They palpate the dorsal surface to locate any prominent bony areas. Imaging tests provide definitive confirmation through detailed views of bone structures. X-rays reveal the exact size and location of projections along joint margins. Advanced scans like CT or MRI offer three-dimensional perspectives when soft tissue involvement requires clarification.
Doctors differentiate these growths from other conditions such as stress fractures or ganglion cysts. They review patient history including activity levels and previous injuries. Blood tests rule out systemic issues like gout that mimic similar symptoms. Functional assessments measure how the foot moves during walking. This comprehensive approach ensures accurate diagnosis and tailored treatment plans. Timely imaging prevents unnecessary delays in care.
Conservative Approaches That Deliver Real Results
Physical therapists guide patients through targeted exercises that strengthen surrounding muscles and improve stability. Calf stretches lengthen tight tissues that pull on the midfoot. Patients perform towel scrunches by gripping fabric with their toes to activate intrinsic foot muscles. Ankle circles enhance joint lubrication and reduce stiffness effectively. These movements promote better blood flow and decrease inflammation naturally.
Orthotics redistribute pressure away from sensitive dorsal areas. Custom inserts support the arch and cushion high-impact zones. Proper footwear choices feature wide toe boxes and flexible uppers that accommodate any prominence. Anti-inflammatory medications ease pain during flare-ups when used as directed. Ice application for 15 minutes several times daily controls swelling after activity. Rest periods allow tissues to recover without constant stress.
A bone spur on top of foot responds well to these non-invasive strategies in most situations. Consistent adherence to home programs yields noticeable improvements within weeks. Patients track progress through pain journals and activity logs. Therapists adjust routines based on individual responses and functional goals. This conservative path restores comfort while preserving natural foot mechanics.
Step-by-Step Exercises for Enhanced Foot Mobility
You begin each session with gentle warm-ups to prepare tissues safely. Sit with legs extended and loop a towel around the ball of your foot. Pull the towel toward your body while keeping the knee straight to stretch the calf and top extensors. Hold for 30 seconds and repeat three times per side. This movement elongates tight structures that contribute to dorsal pressure.
Next you perform marble pickups to strengthen toe flexors. Scatter small objects on the floor and use your toes to grasp and lift them into a container. Complete three sets of 15 repetitions daily. The exercise builds intrinsic muscle support that stabilizes the midfoot during gait. You follow with resisted ankle dorsiflexion using a therapy band. Anchor the band and pull your foot upward against resistance for controlled strengthening.
You incorporate balance work on a foam pad to improve proprioception. Stand on one foot for 30 seconds while maintaining neutral alignment. Progress to eyes-closed variations as confidence grows. These routines enhance overall foot function and reduce reliance on compensatory patterns. Patients who practice daily report fewer pain episodes and greater endurance.
Surgical Solutions for Persistent Cases
Surgeons consider operative intervention when conservative measures fail to provide adequate relief. Arthroscopic techniques remove the bony projection through small incisions with minimal tissue disruption. This approach shortens recovery time compared to traditional open procedures. Patients resume light activities within days under guided protocols.
Postoperative physical therapy rebuilds strength and restores full range of motion. Surgeons address any underlying joint damage simultaneously to prevent recurrence. Success rates remain high when patients follow rehabilitation guidelines closely. The procedure eliminates the mechanical irritation that causes ongoing symptoms. Long-term studies show sustained pain reduction and improved quality of life for suitable candidates.
Proactive Steps to Prevent Future Development
You maintain healthy weight levels to minimize joint loading during everyday movement. Balanced nutrition supports cartilage health through anti-inflammatory foods rich in omega-3s. Regular low-impact activities like swimming preserve flexibility without excessive stress. You select athletic shoes with ample cushioning and replace them before wear patterns develop.
Routine stretching keeps foot muscles supple and reduces tension on dorsal structures. Annual podiatric checkups catch early biomechanical changes before they progress. Custom orthotics correct alignment issues proactively in at-risk individuals. Education about proper form during sports prevents repetitive trauma. These habits create a foundation for lifelong foot health and activity enjoyment.
A bone spur on top of foot becomes less likely when you implement these evidence-based prevention tactics consistently. Community programs teach proper footwear selection and foot care techniques. Employers in standing occupations provide ergonomic supports that lower incidence rates significantly.
Home Remedies and Lifestyle Adjustments for Ongoing Comfort
You apply contrast baths alternating warm and cool water to stimulate circulation and reduce swelling. Epsom salt soaks relax muscles and draw out inflammation after long days. Elevation during rest periods drains excess fluid from the foot effectively. Over-the-counter inserts offer immediate cushioning while awaiting custom options.
Dietary changes emphasize collagen-boosting nutrients that support joint integrity. Hydration maintains tissue elasticity and prevents stiffness. Stress management techniques like yoga improve overall biomechanics by reducing muscle guarding. Supportive socks with targeted compression enhance comfort during travel or work. These simple adjustments complement professional care and empower patients to manage symptoms independently.
Knowing When Professional Help Becomes Essential
You seek immediate evaluation if pain persists despite rest or interferes with normal walking. Sudden swelling accompanied by redness signals possible infection that requires prompt attention. Numbness or tingling indicates nerve compression that specialists must address quickly. Progressive deformity or inability to bear weight warrants urgent assessment.
Podiatrists provide comprehensive care plans that evolve with patient needs. Early consultation prevents minor issues from becoming debilitating conditions. Telemedicine options make access convenient for busy schedules. Multidisciplinary teams including orthopedists and therapists deliver coordinated treatment. Timely intervention restores function and prevents long-term limitations.
A bone spur on top of foot demands attention when symptoms disrupt daily life or athletic pursuits. Specialists equip patients with tools for sustained relief and prevention. Ongoing monitoring ensures optimal outcomes throughout recovery journeys.
Embracing a Pain-Free Future with Informed Care
You now possess detailed knowledge about managing dorsal foot concerns effectively. Consistent application of these strategies transforms discomfort into manageable or eliminated symptoms. Active participation in treatment plans accelerates healing and builds resilience. Support networks connect individuals facing similar challenges for shared encouragement.
Healthcare advancements continue to refine diagnostic and therapeutic options for foot conditions. Patients who stay informed make empowered decisions about their wellness. Regular movement combined with smart footwear choices maintains foot vitality across decades. The journey toward comfort begins with awareness and commitment to proven methods.
This comprehensive approach addresses every aspect of bony growth management on the upper foot. You integrate exercises, lifestyle tweaks, and professional guidance seamlessly into routines. Results compound over time as strength and flexibility improve steadily. Many individuals return to favorite activities with renewed confidence after following structured protocols. Your feet carry you through life’s adventures when you prioritize their health proactively.
READ ALSO: Persistent Runny Nose: Causes, Concerns, and When to Seek Medical Advice
