Knee injuries strike suddenly and sideline active people from their routines. A quick pivot on the basketball court or an unexpected slip on uneven ground forces the joint into an unnatural position. The ligaments stretch or tear under pressure, and swelling follows within minutes. Individuals notice instability that makes walking difficult.
Doctors identify twisted knee symptoms through physical exams and patient reports that highlight the exact moment of injury. Early recognition prevents further damage and speeds recovery. People who ignore initial signs often face prolonged discomfort and reduced mobility. This guide equips readers with clear information on what happens inside the knee, how to spot problems, and steps that restore full function.
What Triggers a Twisted Knee Injury
Athletes twist their knees during high-impact sports like soccer, tennis, or skiing. The foot plants firmly while the body rotates, and the joint absorbs tremendous rotational force. Non-athletes encounter the same mechanism when they step off a curb awkwardly or turn too quickly while carrying heavy loads. Poor footwear, weak thigh muscles, and previous knee issues increase vulnerability.
The anterior cruciate ligament (ACL) bears the brunt of these forces in many cases, while the medial collateral ligament (MCL) suffers when sideways pressure combines with the twist. Meniscus cartilage can also tear simultaneously, complicating the picture. Active individuals strengthen surrounding muscles to absorb shock and maintain proper alignment during movement. Proper warm-ups and technique training reduce the likelihood of these injuries occurring in the first place.
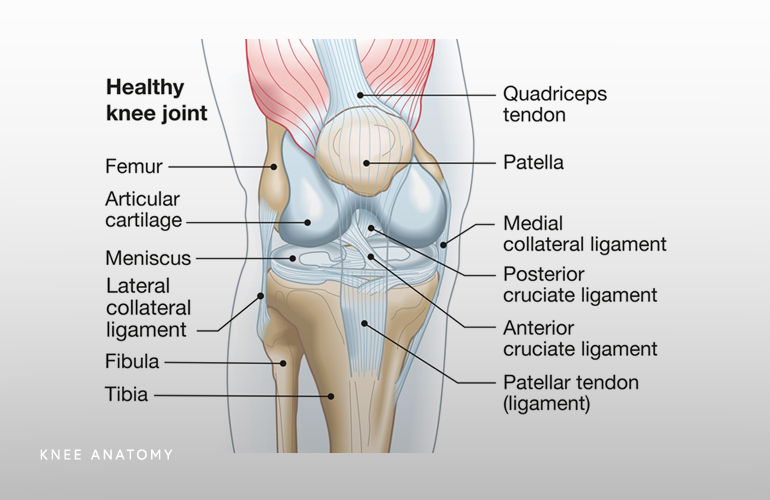
Knee Joint Anatomy That Explains Vulnerability
The knee operates as a hinge joint supported by four major ligaments that provide stability in multiple directions. The ACL prevents the tibia from sliding forward under the femur, while the posterior cruciate ligament (PCL) controls backward movement. Medial and lateral collateral ligaments resist sideways forces. Strong quadriceps and hamstrings work together with these ligaments to keep the joint aligned during dynamic activities.
Cartilage cushions the bones and allows smooth gliding. When a twist occurs, one or more of these structures overloads and sustains damage. Orthopedic specialists map the injury location precisely because each ligament responds differently to stress. Understanding this internal layout helps patients visualize why certain movements create pain and why targeted rehabilitation rebuilds strength in the right areas. Strong supporting muscles act like natural braces that protect the ligaments from future overload.
Recognizing the Primary Signs Right After Injury
Patients feel immediate sharp pain that intensifies with weight bearing. The joint swells rapidly as fluid accumulates inside the capsule. Bruising appears around the kneecap or along the sides within hours. Many people hear or feel a distinct pop at the moment of injury, signaling ligament damage. The knee gives way when individuals try to change direction, creating a sensation of instability. Stiffness sets in quickly and limits the normal range of motion.
These signs vary in intensity depending on whether the sprain is mild, moderate, or severe. Doctors classify injuries into grades that guide treatment decisions. Grade one involves minor stretching with little swelling, while grade three represents a complete tear that requires more aggressive intervention. Twisted knee symptoms manifest differently in each person, yet the pattern of pain, swelling, and instability remains consistent across cases.
Additional Indicators That Demand Attention
Beyond the obvious swelling and pain, individuals report tenderness when they press specific points around the joint. The knee locks or catches during movement if meniscus damage accompanies the twist. Numbness or tingling down the leg sometimes occurs when swelling compresses nearby nerves. Athletes notice reduced power in the quadriceps, making it hard to straighten the leg fully. Bruising that spreads down the calf indicates possible deeper vascular involvement.
These secondary signs help differentiate a simple sprain from more complex damage that involves multiple structures. Physical therapists assess gait patterns and balance to quantify the extent of functional loss. Patients who experience these indicators seek evaluation sooner because delays allow scar tissue to form and complicate later recovery. Consistent monitoring of all changes ensures comprehensive care that addresses every aspect of the injury.
Timing Matters: When to Consult a Medical Professional
Individuals contact orthopedic specialists immediately when they cannot bear weight or when the knee buckles repeatedly. Severe pain that wakes them at night or swelling that does not respond to basic rest signals the need for imaging. Persistent instability after 48 hours of conservative care also warrants professional assessment. Doctors perform stress tests that reveal ligament laxity and order X-rays to rule out fractures.
MRI scans provide detailed views of soft tissue damage that plain films miss. Early intervention prevents chronic issues like arthritis or recurrent instability. Patients who wait often require more invasive procedures later. Healthcare providers emphasize that timely evaluation leads to better outcomes and shorter rehabilitation periods. Families encourage loved ones to act quickly because ignoring the problem rarely resolves on its own.

Diagnostic Steps Specialists Follow
Orthopedists begin with a thorough history that captures the exact mechanism of injury and immediate sensations. They conduct physical exams that include the Lachman test for ACL integrity and valgus stress tests for MCL stability. Imaging confirms suspicions and rules out bone involvement. Ultrasound offers a quick, radiation-free look at fluid and superficial structures in some clinics.
Specialists compare both knees to identify subtle differences in range and strength. Blood tests occasionally check for underlying inflammatory conditions that slow healing. Accurate diagnosis directs the treatment plan and sets realistic expectations for recovery timelines. Patients participate actively by describing symptoms clearly, which helps clinicians pinpoint the exact structures involved. This collaborative process ensures the chosen interventions target the root cause rather than just surface discomfort.
Proven Treatment Options That Promote Healing
Doctors prescribe rest immediately after confirming the injury to protect damaged tissues. Ice applied for 15 minutes every few hours reduces swelling and numbs pain. Compression wraps limit fluid buildup while elevation drains excess fluid through gravity. Over-the-counter anti-inflammatory medications ease discomfort in the first week. Physical therapists introduce gentle range-of-motion exercises once acute swelling subsides.
Bracing stabilizes the joint during daily activities and prevents re-injury. Severe tears often require surgical reconstruction using grafts that replace torn ligaments. Arthroscopic techniques minimize incision size and speed return to function. Post-surgical protocols include progressive strengthening that rebuilds muscle support around the new graft. Patients follow structured programs that advance only when milestones are met, ensuring safe progression.
Home Care Techniques You Can Start Today
People apply the RICE protocol at home to manage initial inflammation effectively. They remove compression wraps periodically to check skin circulation and prevent constriction. Gentle ankle pumps promote blood flow without stressing the knee. Over-the-counter creams containing menthol provide localized relief between icing sessions. Nutrition plays a key role as patients increase protein intake to support tissue repair and consume anti-inflammatory foods like berries and fatty fish. Hydration keeps joint fluid healthy and aids overall recovery.
Individuals track daily pain levels in a journal to identify patterns and adjust activities accordingly. Consistent elevation during the first 72 hours dramatically reduces swelling and shortens the acute phase. These simple steps empower patients to take control while awaiting professional follow-up appointments.
Smart Prevention Strategies for Active Lifestyles
Athletes incorporate balance exercises into warm-ups to improve proprioception and reaction times. Strength training focuses on quadriceps, hamstrings, and glute muscles that stabilize the knee during twists. Proper footwear with adequate support prevents excessive foot rotation on various surfaces. Coaches teach landing techniques that emphasize soft knees and aligned hips. Regular flexibility routines maintain muscle length and reduce tension across the joint.
Individuals with previous injuries wear supportive braces during high-risk activities. Weight management reduces load on the knees and lowers injury risk significantly. These proactive measures build resilience that protects the joint through years of activity. Communities that emphasize injury prevention see fewer long-term knee problems among participants.
Rehabilitation Exercises That Restore Full Function
Physical therapists guide patients through quad sets that activate the front thigh muscles without moving the joint. Heel slides improve flexion gradually while maintaining control. Straight-leg raises strengthen the quadriceps in a safe position. Wall squats build endurance once basic strength returns. Balance boards challenge stability and retrain neuromuscular pathways. Therapists progress patients to single-leg exercises that mimic real-life demands.
Resistance bands add controlled load that builds power safely. Patients perform these movements daily with proper form to avoid compensation patterns that lead to secondary issues. Consistency accelerates return to sports and daily activities. Follow-up assessments measure progress objectively and adjust programs accordingly.

Long-Term Outlook and Lifestyle Adjustments
Most people regain full knee function within three to six months when they follow recommended protocols diligently. Surgical cases may extend to nine months for complete return to high-level sports. Ongoing strength maintenance prevents re-injury and supports joint health into later years. Patients adopt lifelong habits that include proper warm-ups and cross-training to avoid overuse.
Regular check-ups catch minor issues before they escalate. Many individuals report greater knee awareness after recovery, which improves overall movement quality. Supportive communities and online resources provide motivation during challenging phases. The journey from injury to full strength teaches valuable lessons about body mechanics and resilience. Active people emerge stronger and more knowledgeable about protecting their joints.
Doctors identify twisted knee symptoms early when patients describe the injury mechanism accurately. Rehabilitation specialists address twisted knee symptoms with customized programs that target specific weaknesses. Families learn to recognize twisted knee symptoms so they can support loved ones effectively.
Coaches incorporate education about twisted knee symptoms into team training sessions. Researchers continue studying twisted knee symptoms to develop better prevention tools. Healthcare providers emphasize that understanding twisted knee symptoms empowers individuals to act decisively. Everyone benefits when communities share knowledge about twisted knee symptoms openly. This collective awareness reduces the impact of knee injuries across all age groups.
READ ALSO: Bone Spur on Top of Foot: Causes, Signs, and Best Treatment Options
